Cognitive disengagement syndrome (sluggish cognitive tempo)
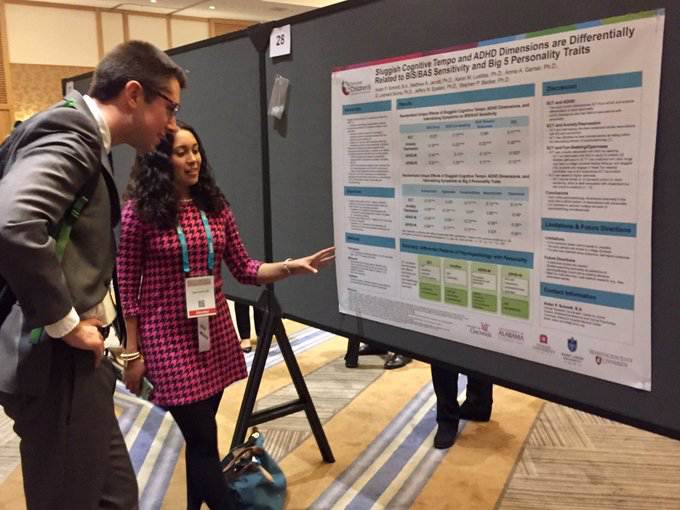
It is increasingly clear that there is a subset of children who display a unique pattern of attentional difficulties that are not captured by attention-deficit/hyperactivity disorder (ADHD). This cluster of attentional symptoms is termed “cognitive disengagement syndrome” (CDS; previously called sluggish cognitive tempo; Becker, Willcutt et al., 2022) and includes excessive daydreaming, confusion, seeming to be ‘in a fog,’ and slowed behavior/thinking. I was first introduced to the CDS construct while examining co-occurring ADHD and internalizing symptoms during graduate school. Since that time I have established a programmatic line of research examining whether CDS is not only distinct from other mental health symptoms but also differentially or uniquely associated with youths’ functioning. I have demonstrated that although CDS is associated with higher rates of ADHD inattention, depression, anxiety, and daytime sleepiness, CDS is nonetheless statistically distinct from these domains. My research has also led to some of the first studies showing that CDS symptoms are associated with both academic impairment and social problems, even after controlling for ADHD symptoms. My colleagues and I have also conducted longitudinal research demonstrating CDS to predict later impairment. My research continues to examine the internal and external validity of the SCT construct across the life span. My research in this area is supported by the National Institute of Mental Health (K23MH108603, R01MH122415) and the Institute of Education Sciences (R305A160064, R305A200028).
Sleep in teens with and without ADHD
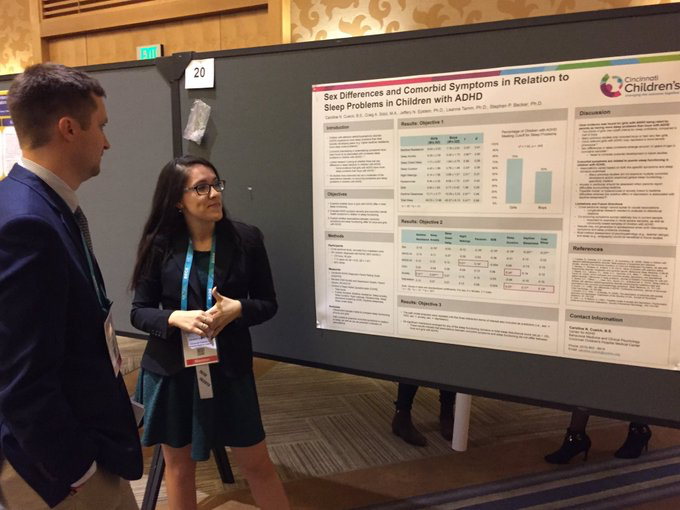
Sleep plays a crucial role in youths’ daily functioning and youth with ADHD experience more sleep problems than their peers. This fact became especially salient to me while I was completing a rotation in the CCHMC Behavioral Sleep Medicine Clinic during my final year (internship) of doctoral training. Since that time, I have conducted a series of studies documenting a strong association between sleep problems and poorer attention in healthy children as well as children with sleep disorders. In addition, I conducted the first study showing sleep problems to predict increased oppositional and depressive symptoms one year later in adolescents diagnosed with ADHD, even after controlling for initial levels of depression and oppositionality. My colleagues and I have also found that sleep problems are associated with academic problems and internalizing symptoms in older adolescents diagnosed with ADHD. As the lead-guest editor for a special issue on sleep in adolescence for the Journal of Youth and Adolescence, I conducted a substantive review in advancing a biopsychosocial model for the study of sleep in adolescence. In this review, my co-authors and I noted a clear gap between observational studies conducted to date that have identified correlations and experimental studies yet to be conducted that can better speak to causality. We recently completed the first experimental sleep restriction/extension study in adolescents diagnosed with ADHD, with findings showing shortened sleep duration to be causally linked to poorer attention, increased sleepiness, and more oppositional and mood problems. My colleagues and I are currently conducting longitudinal research to understand how sleep problems impact the academic and socio-emotional adjustment of teens with and without ADHD as they transition from middle school to high school. The long-term goal of this research program is to better understand the interrelations between ADHD, sleep, and impairment, as well as to examine sleep as a potential target for intervention in adolescents with ADHD. My research in this area is funded by an R03 from the National Institute of Mental Health and an exploration grant with Dr. Joshua Langberg (Virginia Commonwealth University) from the Institute of Education Sciences (R305A160126).
Co-occurrence of ADHD and internalizing symptoms
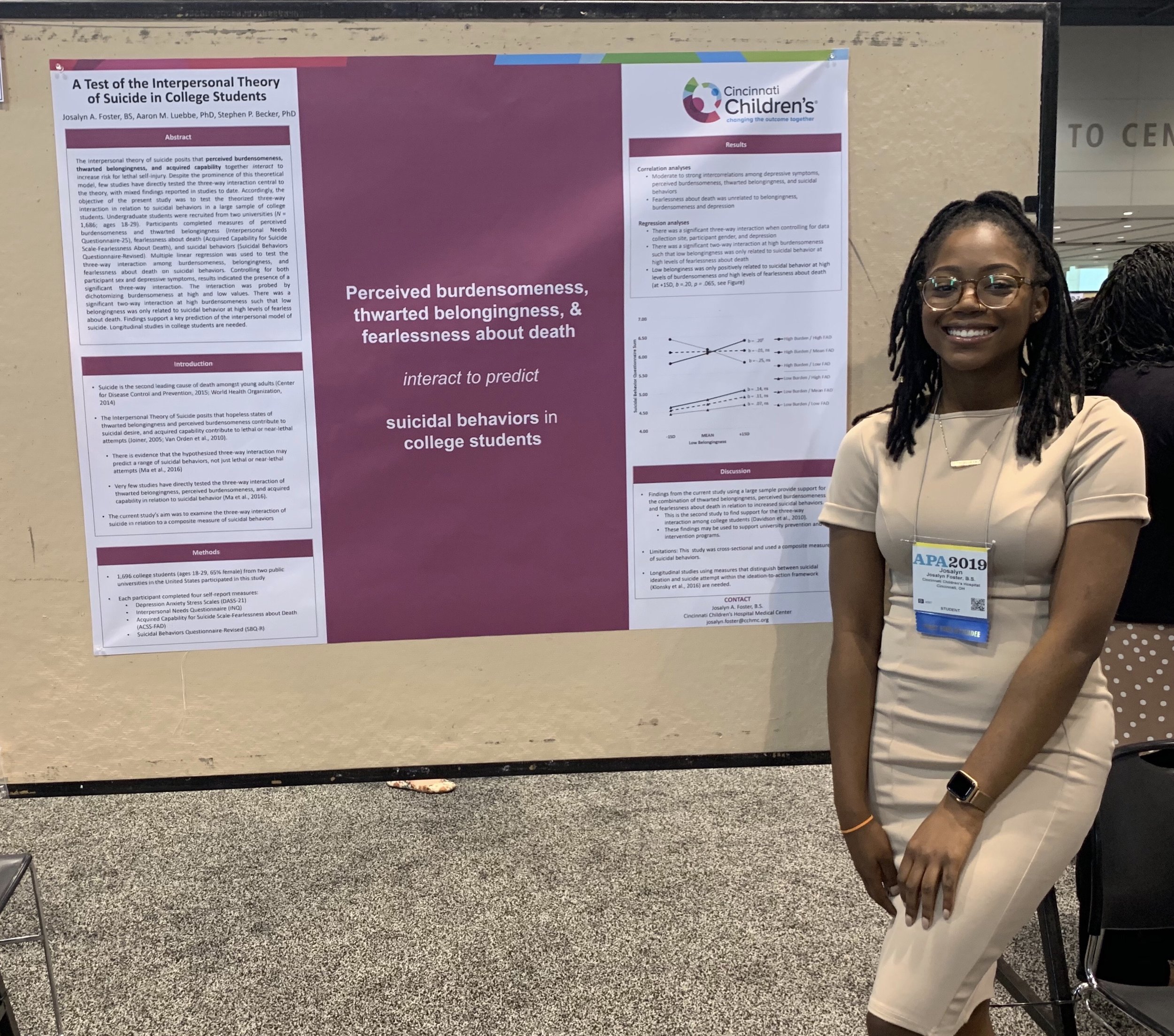
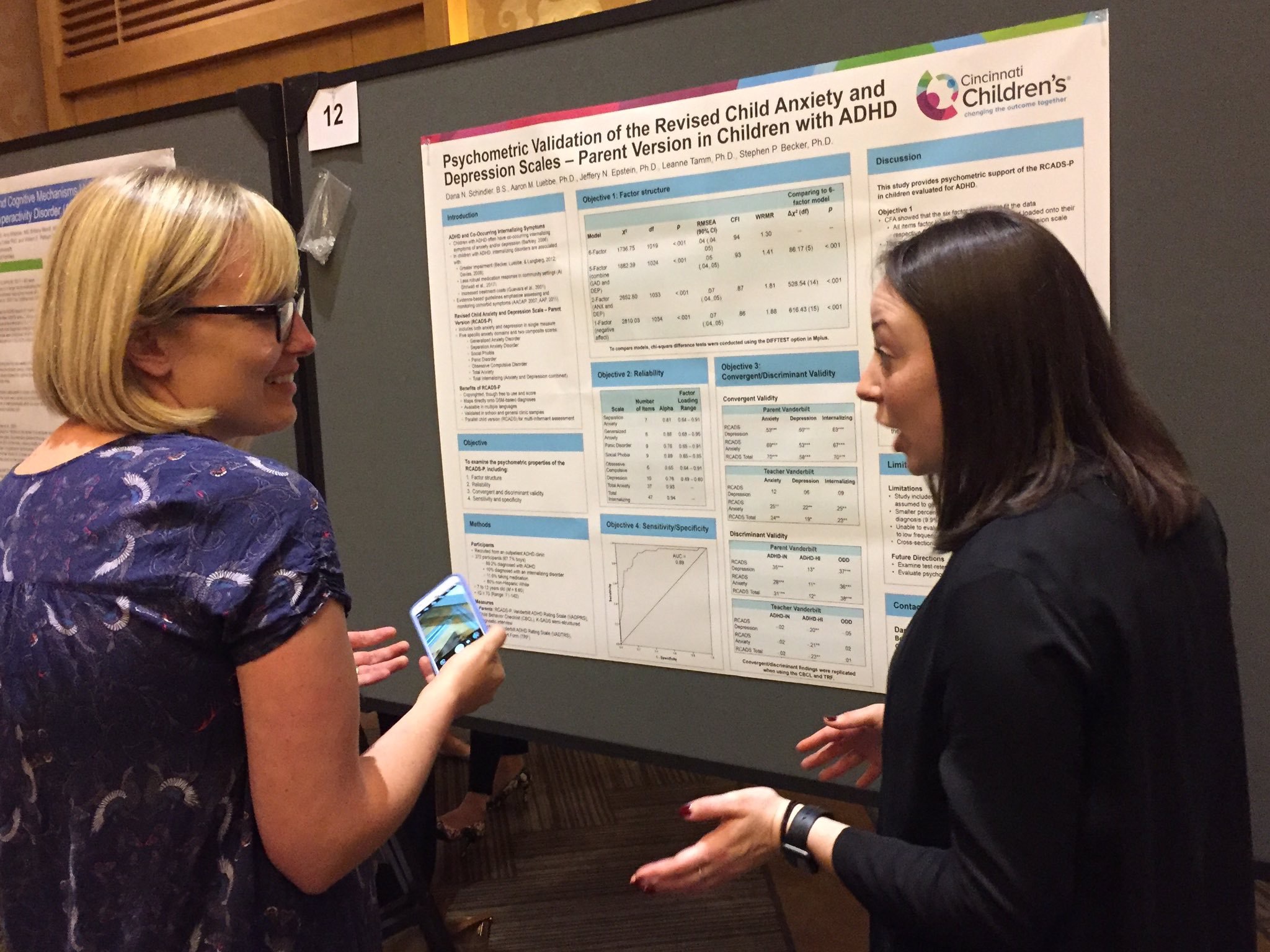
Children with ADHD frequently experience comorbid mental health problems. Although psychiatric comorbidity may exacerbate the impairments experienced by children with ADHD, much more research has focused on externalizing rather than internalizing comorbidities. To address this gap in the literature, I have conducted a systematic review and led several studies to help further our understanding of how internalizing symptoms affect the relation between ADHD and social adjustment. These studies have shown that depressive symptoms (and anhedonia in particular) may be more detrimental in terms of the social functioning of youth with ADHD, especially in adolescence. Also, it is likely that internalizing and peer problems are transactional in nature, and the association between peer problems and internalizing in children with ADHD may be stronger for girls than for boys. My research in this area aims to further our understanding of internalizing symptoms in children with ADHD and the extent to which these co-occurring symptoms contribute to social and academic impairments.
I have a long-standing interest in school-based interventions for youth with ADHD. School-based mental health is a promising and important area for addressing children’s mental health needs. My work in this area started in my first year of graduate school in the Miami University Center for School-Based Mental Health and continues to this day. I have been involved in all aspects of treatment development research, including examining how students with emotional and behavioral disorders are initially referred and assessed, refining interventions for implementation by school mental health providers, efficacy research, and identification of mediators of treatment gains. In particular, I worked extensively in the refining and evaluation of two school-based interventions for young adolescents with ADHD, the Challenging Horizons Program (CHP) and the Homework, Organization, and Planning Skills (HOPS) interventions. I am especially interested in identifying moderators and mediators of treatment efficacy and effectiveness. In addition, we are currently conducting a pilot open trial of a cognitive-behavioral sleep intervention for adolescents who have both ADHD and sleep problems.
Interventions for youth with ADHD
My three scientists-in-training!